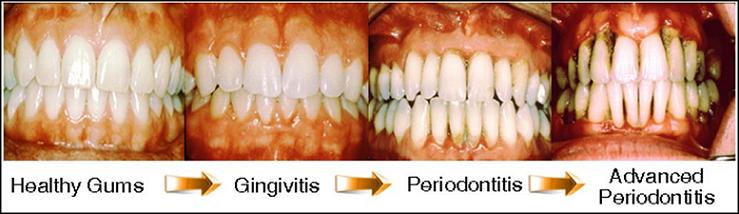
Want to avoid gum surgery and use a gingivitis treatment at home? Discover how to cure gingivitis naturally without harsh chemicals and their side effects.
There are natural solutions that can help avoid deep cleanings due to plaque and tartar.
There is no shortage of people who desperately want to know how to treat gingivitis at home without harsh chemicals. Gingivitis is health problem that affects around two-thirds of the adult population. It can range from being a mild oral health condition, to causing long-term dental problems. Fortunately, for those who develop the condition, there is effective gingivitis treatment that can be recommended by your dentist.
Your dentist is generally able to spot the signs of gum disease before you will. This is one of the reasons it is so important to visit your dentist twice each year for a check-up. If they notice the tell-tale signs of the condition, they can suggest appropriate treatment that will restore your gum health quickly.
Symptoms of Gingivitis
There are various symptoms that you may begin to notice if your oral health is not optimal and gingivitis has begun to develop. Be vigilant for the early warning signs of gingivitis and you can boost your dental health by identifying and reversing the condition early on, before long-term damage can occur.
Some of the initial stages of gingivitis may include:
- Bleeding gums when you brushing your teeth
- Redder than usual gum tissue
- Sore or inflamed gums
- Bad breath, even after you have brushed your teeth
- Bad taste in your mouth.
If the condition is diagnosed at this stage and you begin to treat the condition and follow an effective oral health program, then you can easily reverse the condition and restore your dental health. However, if the condition is allowed to develop, then you may begin to observe more acute symptoms, which can include:
- Receding gums
- Wobbly teeth
- Dental pain
- Tooth loss
- Severe infection of the gum tissue.
When gingivitis becomes advanced, it is generally known as periodontitis. Once the condition has reached this stage, it generally requires much more intensive treatment. This may require dental surgery and potentially expensive and painful procedures to eradicate diseased tissue and infection.
Is Gingivitis Contagious?
No, not in the way we think of a virus. However, the cause of gingivitis can spread in your gum and teeth, possibly entering you bloodstream where it can wreak havoc on your health. It can be deadly!
What is the cause of gingivitis?
What Causes Gingivitis?
 Gum disease is almost always caused when bacteria and plaque build up on the gum tissue and teeth. This occurs when the bacteria that form on your teeth and gums daily after eating is not removed effectively. When you eat, the food residue left behind encourages bacteria, which feed on the leftover food.
Gum disease is almost always caused when bacteria and plaque build up on the gum tissue and teeth. This occurs when the bacteria that form on your teeth and gums daily after eating is not removed effectively. When you eat, the food residue left behind encourages bacteria, which feed on the leftover food.
The bacteria flourish after each time you eat and must be removed through brushing, flossing and using a mouthwash as part of an effective dental hygiene routine. If they are not removed effectively, then the bacteria will begin to cause infection.
Bacteria react with your saliva and then cause a substance known as plaque to develop. This is a yellowish, sticky substance that clings to your teeth and gums and causes the infection. Over time, if the plaque and bacteria are not removed, the infection will become more advanced and develop into gingivitis.
6 Factors that influence gum health
Following a thorough home dental hygiene routine is vital if you want to keep your teeth and preserve your gums. However, there are other factors that increase your chances of developing gingivitis or exacerbate the condition. Some of these factors include:
- Smoking – smoking leaches your body of vitamin C, which is needed for healthy circulation and healthy tissue. When you smoke, deposits of tar stay on your teeth and gums, which also damages the gum tissue.
- Diet – if you eat a diet that is high in sugar, then you are opening the door to gingivitis. The bacteria that cause gingivitis love to feed on sugar. You should therefore, limit the amount of sugar that you are consuming each day. Eating a lot of processed foods also limits the amount of vitamins and nutrients that can protect your oral health. Try to cut down on sugary, fatty and processed foods and eat more fresh fresh vegetables instead.
- Water – it is important that you are drinking between six and eight glasses of water a day to keep your body healthy. Drinking the appropriate amount of water will also help to flush bacteria from your mouth.
- Hormonal upheavals – women are slightly more likely to develop gingivitis and other oral health conditions thanks to hormonal changes. Fluctuations of hormones particularly during pregnancy and menopause can cause gingivitis to occur.
- Other Serious health conditions – there are certain health conditions that can make you more susceptible to developing gingivitis. Some conditions such as diabetes, heart disease and many others may affect your ability to fight off bacterial infections.
- Medications – there are also some medications that can make you more likely to develop gingivitis or other gum disease. If you take a medication regularly, you should talk to your doctor or dentist about whether it may affect your gum health and how you can protect it from bacterial infection.
What do I do if I have developed gingivitis?
If you think you may have developed gingivitis, the first thing you should do is to visit your dentist. They are able to make a proper diagnosis and suggest a treatment that will ease your individual symptoms most effectively.
Fortunately, if you catch the condition early on, before it becomes periodontitis, you can reverse gum disease and restore your total oral health. There are some simple steps that you can take in order to get rid of the infection and enjoy good oral health once again.
- Brush after every meal each day – ideally, you will clean your mouth each time you eat. If you have already developed gingivitis, then this is a necessary step in order to get the bacteria levels under control in your mouth. Brushing is the most effective way to eradicate oral bacteria. Once you have reversed the condition, you can get by on brushing twice a day.
- Floss between teeth to remove residual food particles and bacteria. Buy dental tape and use it daily to get rid of the extra muck that gets stuck between your teeth when you eat. Flossing gets rid of the leftovers in areas where your toothbrush can’t reach. Consider using a water floss, which is very effective.
- Use a mouthwash – Using a chemical-free mouthwash or equivalent to swill around your mouth twice a day will help to flush out the extra bacteria that are left behind after brushing and flossing. Natural essential oils for gingivitis mixed together with water in the mouth may work well.
With these three simple steps, you can often ward off early stage gingivitis.
Your dentist may suggest other treatment if they consider that your gum disease has advanced to a point where following a good oral hygiene routine is not enough.
What Products Should I Use?
It is important to choose appropriate products to use as well as following an appropriate dental hygiene routine. There are many products for sale that can actually damage your gum health rather than supporting it. There are certain ingredients that you want to avoid:
No Sodium Lauryl Sulphate (SLS): One of the key ingredients to avoid is sodium lauryl sulphate. This chemical is commonly used in toothpaste as well as shampoos, beauty products and cleaning products. It is a foaming agent, but it can hurt sensitive gums and is best avoided. Look at the ingredients of any product you are considering buying and ensure that it does not contain SLS.
No Flouride: Fluoride has long been added to toothpaste as it is thought to strengthen teeth. Many studies have now shown, however, that it is highly toxic and may also have limited benefit to teeth. It is, therefore, best to avoid dental products that contain this ingredient.
No Alcohol: Alcohol is sometimes included in mouthwashes, but you should try to avoid buying products that contain it. This ingredient can dry out your mouth, which is a problem as saliva protects your mouth from the bacteria that can cause gingivitis.
It is often best to purchase products that contain natural ingredients. These days there are some very effective commercially available products that are natural. They do not contain any potentially damaging ingredients. Some of the natural herbs that can effectively clean and protect your teeth and gums include:
- Tea tree oil – tea tree oil has been used by Australian aborigines for thousands of years for its antiseptic, antibacterial and anti-fungal properties. This ingredient is particularly helpful for eradicating the bacteria that harm your gum health.
- Peppermint essential oil– peppermint eradicates bacteria and leaves your mouth feeling clean and fresh. Some formulas are combined with spearmint and almond oils and in the right combination are alone sufficient to be a very potent solution to kill and control bacteria. Here is an example of one powerful formula that works.
- Aloe vera – reduces redness and swelling of gums and soothes the mouth.
- Neem – neem has also been shown to be able to get rid of bacteria and plaque inside the mouth. It can also prevent cavities and keep the mouth feeling fresh and clean.
Using the Right Technique
By following a stringent oral health routine at home where you brush, floss and rinse at least twice a day and choosing the right dental products, you can generally reverse the early stages of gum disease. However, you should also ensure that you are using the right technique so that you can remove the bacteria and plaque efficiently. Using the correct technique will also ensure that you do not injure your sensitive gums, which can also encourage oral infection.
Brushing
When brushing your teeth there is a specific technique to use. A thorough brushing should take around two minutes, which is much longer than most people spend. Make sure to cover the upper teeth and the lower teeth, on the inside, outside and chewing surfaces.
Make sure you give extra attention to the hard to reach areas at the back of your mouth and to any fillings or other dental work that you may have. Hold your toothbrush at a 45 degree angle and use short strokes moving away from the gums. Always use a soft-bristled brush as harder brushes can easily damage gums and tooth enamel.
Flossing
When flossing, grab a piece of floss or dental tape that is around 30 centimetres long.
- Wind some of the floss around your index finger, leave about 5 centimetres and then wind the floss around your other index finger.
- Start with your top teeth at the back and work forwards.
- Place the floss gently in the groove between the teeth then delicately move the floss up and to the side of one tooth and then to the other. Each time you should be creating a C-like patter with the floss around the tooth.
- Repeat with each gap between teeth at the top of your mouth and then with the bottom teeth.
Rinsing
Using a mouth rinse is reasonably straightforward. Always follow the directions on the mouth rinse that you purchase, but in general, you need to swill it around your mouth for around 45 seconds. This is usually long enough to get to the hard to reach areas and flush out any bacteria that may still be hiding there after brushing and flossing.
If you follow a good daily oral hygiene routine, you are likely to be able to avoid developing cavities, gum disease or other dental problems. Good oral health is also linked to good overall health in adults, so it pays to make the health of your gums and teeth a priority.
If you do develop gum disease, it is important that you seek out gingivitis treatment at home early on to avoid having to deal with advanced dental health problems that can be time consuming, costly and even painful. Do not put off investing in quality products, but be sure they are natural and free of irritating ingredients that could cause more long-term harm than good.
What are you waiting for? Learn how to get rid of gingivitis naturally.
Click here to learn more about a proven gingivitis treatment at home used by many with success.